Newsletter December 2015
Here we are with our Newsletter once again. There’s been plenty happening so first, let’s tell you about our research work and how your money is being spent.
First, protein control.
 Much has been happening at St George’s University of London in Tooting. Dr. Androulla Elia’s team- she’s on the far right with Ricky Henry-Grant in the middle and Charlotte Adiseshiah – has continued to research the control of proteins in fighting pancreatic cancer. We could get very technical here, but suffice to say that a protein known as “4E-BP1”, which is involved in controlling the mechanism under which cells make all other proteins, is often present in very low amounts in pancreatic cancer cells. Ways of enhancing the production of this protein are being explored to determine if this makes tumour cells more likely to die. So far it has been shown that the treatment of pancreatic cancer cells with a combination of the drug Gemcitabine and TRAIL, a hormone-like chemical produced naturally by the body, creates a dramatic increase in the level of 4E-BP1, which is itself caused by the activation of other proteins which are involved in killing cancerous cells. It has also been seen that there is a decrease in the activity of a protein known as “mTOR”, which regulates 4E-BP1 and this is being further investigated. It is gratifying to see that the hard work of the team is being rewarded despite the fact there is still a long way to go.
Much has been happening at St George’s University of London in Tooting. Dr. Androulla Elia’s team- she’s on the far right with Ricky Henry-Grant in the middle and Charlotte Adiseshiah – has continued to research the control of proteins in fighting pancreatic cancer. We could get very technical here, but suffice to say that a protein known as “4E-BP1”, which is involved in controlling the mechanism under which cells make all other proteins, is often present in very low amounts in pancreatic cancer cells. Ways of enhancing the production of this protein are being explored to determine if this makes tumour cells more likely to die. So far it has been shown that the treatment of pancreatic cancer cells with a combination of the drug Gemcitabine and TRAIL, a hormone-like chemical produced naturally by the body, creates a dramatic increase in the level of 4E-BP1, which is itself caused by the activation of other proteins which are involved in killing cancerous cells. It has also been seen that there is a decrease in the activity of a protein known as “mTOR”, which regulates 4E-BP1 and this is being further investigated. It is gratifying to see that the hard work of the team is being rewarded despite the fact there is still a long way to go.
Elsewhere in St George’s, Professor Gus Dalgleish’s team continue to study the effects of various combinations of drugs on cancerous cells. They have been fortunate to recruit a researcher from the Institute of Cancer Research who brings with him extensive research skills and who is now recruiting a research postgraduate to further strengthen the team. This team will continue to research the benefits of combining the drug Gemzar with a non-specific vaccine, IMM-101, and with a vitamin D3 supplement, a combination which has shown a distinct survival advantage over Gemzar alone. This was derived and executed on the back of our research into Gemcitabine. This combination is unique in that it is non-toxic and is inexpensive to produce. Other drugs that are non-toxic and may enhance the anti-cancer effects, which we are starting to research in combination, include the cannabinoids, the anti-malarials and low dose Naltrexone.
At Imperial College, London, Mr Adam Frampton, whose research we have partly funded, has continued his work to discover novel molecular biomarkers (indicators) for pancreatic cancer. As Adam says, pancreatic cancer is often detected too late, resulting in many patients being ineligible for surgery. Several small indicators have been identified in endoscopic biopsies from patients with suspicious pancreatic lesions that could be used to aid diagnosis, as they are stable, easily measured and can improve biopsy accuracy. This study is currently under review by the respected journal Oncotarget.
The team is also looking at indicators in the bile from patients with benign and malignant pancreatic tumours to see if these indicators can distinguish different types of lesion.
All this is further good news as it shows that approaching the problem of pancreatic cancer from different angles may help us get answers quicker than with a single approach.
So what have our tireless supporters been doing?
 In October, Toni Kane ran the 5K in the Bournemouth Marathon Festival of Speed in just under 29 minutes.
In October, Toni Kane ran the 5K in the Bournemouth Marathon Festival of Speed in just under 29 minutes.
This is Toni looking well refreshed after her run.
Toni- many thanks for all your efforts and for the donations you raised.
(The Bournemouth Festival is organised by GSI Charity Central who arrange running events in various parts of the UK. If you would like to participate in any of their events, details are on their web site at gsicharitycentral.com. We are happy to pay for your entry but we do expect you to support our Fund!).
Jonathan Dunnett did it!
As we mentioned in our Summer Newsletter, Jonathan (Jono) Dunnett windsurfed around Britain between mid-June and end September in aid of pancreatic cancer and a charity supporting Tanzanian Orphans and Widows (STOW). This is what Jono had to say;
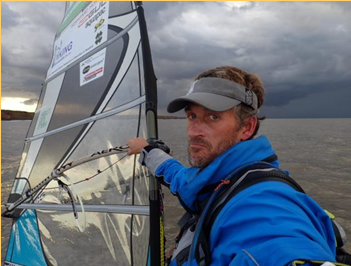 “On my travels I met scores of people. Many approached me upon learning (or observing, from the stickers on my sail) that I was supporting pancreatic cancer research, and very many of these had a personal story of loss to tell, as a result of the disease. As I was sailing around Britain I felt the combined weight of responsibility that I was sailing not just for Paco (the father in a family who treated Jono as their own) but for all those who have lived or are living with their own pancreatic cancer tragedy. It was a responsibility I felt honoured to carry.
“On my travels I met scores of people. Many approached me upon learning (or observing, from the stickers on my sail) that I was supporting pancreatic cancer research, and very many of these had a personal story of loss to tell, as a result of the disease. As I was sailing around Britain I felt the combined weight of responsibility that I was sailing not just for Paco (the father in a family who treated Jono as their own) but for all those who have lived or are living with their own pancreatic cancer tragedy. It was a responsibility I felt honoured to carry.
In early 2015, after I had announced the expedition, another family friend succumbed to the disease. Dennis was an intrepid sailor, and together (when I was a child) we had once sailed round the Lizard peninsula. It was a special moment to sail round there again. There were big seas and the light was failing and in truth I was in a bit of a fix. Dennis would have appreciated that adventure. Most days held adventure, and on many days progress at sea seemed slow or non-existent. Sometimes the wind would become so light that sailing became impossible. Usually I would be some way offshore of a cliff-lined coast, and the water state would be most uncomfortable. Visibility was often poor – land just a shadow through the mist. It was lonely and time passed slowly. From a psychological perspective these times were difficult to live with, but they were also times of personal growth. Through repetition, I learned to trust that difficult times always have an end. That something – eventually – always changes: to see you through, get you home, or get you on your way.
Pancreatic cancer is a difficult problem with no obvious solution, but my experiences renewed my faith that a way around this cruel disease will be found. Good luck RBPCR and strength to those struggling at the moment with their own difficulties”.
More about Jono’s journey is available on the expedition blog: http://www.windsurfroundbritain.co.uk/blog.
Sincere thanks to Jono from all of us at The Ralph Bates Fund for his tremendous support. He generated a fantastic amount in donations and put his own life at risk in doing it. Well done and please don’t forget us when you do it again!
 In May, Emma Keele – on the left- ran the Hackney Half Marathon completing the run in 2 hours 18 minutes which is pretty good for a first timer!
In May, Emma Keele – on the left- ran the Hackney Half Marathon completing the run in 2 hours 18 minutes which is pretty good for a first timer!
Emma is an actress and has appeared in TV series such as “New Tricks”, “Coronation Street”, “Doctors” and the popular “Downton Abbey”.
To be honest, we missed including Emma’s photograph in the Summer Newsletter and hope this entry makes up for the omission!
That’s Emma on the left at the end of the race. It looks as though the person behind has taken a tumble but let’s hope not! Thanks Emma, for your hard work and support.
 And here’s our own Virginia Bates sandwiched between fellow Trustee John Glees, complete with baseball cap on the left and the artist Nigel Stefani, who recently held his first show at The Old Truman Brewery, East London. Titled ‘Conversation’, Nigel works in pencil and graphite on paper and is generously making a donation to our Fund from sales of his work.
And here’s our own Virginia Bates sandwiched between fellow Trustee John Glees, complete with baseball cap on the left and the artist Nigel Stefani, who recently held his first show at The Old Truman Brewery, East London. Titled ‘Conversation’, Nigel works in pencil and graphite on paper and is generously making a donation to our Fund from sales of his work.
 This is one of Nigel’s works- of Virginia. You can view his work at http://nigelstefani.tumbir.com.
This is one of Nigel’s works- of Virginia. You can view his work at http://nigelstefani.tumbir.com.
There was a very interesting and easily-read article in the Daily Telegraph recently regarding pancreatic cancer. We’ve reproduced the article on page 5- text only – but it’s important to mention the following here, which are all worth bearing in mind. It’s worth spreading the word as there is a high level of ignorance about pancreatic cancer.
The symptoms of pancreatic cancer;
Yellow skin or eyes and /or itchy skin.
Unexplained weight loss.
Tummy pain, especially at the top of the abdomen, which may radiate to the back.
Bowel changes such as oily, floating faeces.
Does lifestyle play a part?
About a third of pancreatic cancers are linked to lifestyle. The two main risk factors are obesity and smoking followed by high consumption of alcohol and red and processed meats.
People with type 1 and 2 diabetes have double the risk of developing pancreatic cancer.
The complete article, including pictures can be seen at; http://www.telegraph.co.uk/wellbeing/health-advice/why-pancreatic-cancer-is-the-hidden-killer/
Many thanks to Anna MaGee, the Daily Telegraph feature writer, for providing this link.
On a disappointing note, it was reported recently that NICE, (The National Institute for Health and Care Excellence) has decreed that the drug Abraxane, the only new pancreatic cancer drug licensed for 17 years, will not be funded for victims of pancreatic cancer in England. Those in Wales and Scotland will still be able to benefit. Abraxane, given with the drug Gemcitabine, has been shown to double life expectancy in some cases and to double the two year survival rate. This is distressing news for patients and their families in England, especially as survival rates for pancreatic cancer have not improved over the last 40 years or so. A Clinical Medical Oncologist in London commented; “As oncologists, we struggle to see the rationale for this in an area of high unmet need. With sufferers facing a poor prognosis once diagnosed, it is vital that regulatory bodies address their review systems to take into account the benefit which medicines may bring to people affected with metastatic pancreatic cancer”.
Absolutely right. It goes to show how important research is, into ways to combat pancreatic cancer with inexpensive drugs.
There’s been further media comment recently about charities not spending enough of their income on charitable causes. We’re not here to criticise what others do, but we are proud of the fact that over the twelve years to 31 March 2015, our Fund has spent 98% of all income on charitable activities. None of the Trustees is remunerated and none claim expenses. And as you can tell from this Newsletter, we don’t spend your hard earned donations on fancy glossy leaflets.
We now have a Memorials section on our web site.
If you would like to record something in memory of a loved one including a small photograph if you wish, email the photo and text to us (see email address on page 1) and we’ll post it on our web site.
Many thanks to all our donors- we couldn’t do it without you! Have a healthy and prosperous 2016.
The Trustees.
December 2015.
********************************************************************************
Daily Telegraph article November 30 2015.
Why pancreatic cancer is the hidden killer.
“Have you been in the sun?’ The doctor asked Ivan McMinn. He was there for the intense skin itching he’d had but the medic was more concerned with his jaundiced appearance. ‘She sent me immediately to Accident and Emergency.’
Ivan remembers the day because it was Armistice day, 2011. ‘I looked at my watch and it was 11 minutes past 11 on the 11th of the 11th, 2011. That still gives me goosebumps’. At A&E Ivan, 53 and a father-of-two from Belfast, was asked to stay in hospital for tests. Doctors suspected he may have gallstones, but two days later, he was told he had a cancerous tumour at the head of his pancreas.
Each year, some 8800 people are diagnosed with pancreatic cancer in the UK – one every hour. The illness that claimed the lives of Steve Jobs and actor Patrick Swayze (Sir John Hurt was diagnosed with it in June this year) is currently the fifth most common cause of cancer death in Britain and by 2030 is set to overtake breast cancer as the nation’s fourth largest cancer killer.
In fact, the lack of awareness among both the public and doctors (a recent study found three quarters of Britons couldn’t name a single symptom) and a desperate shortage of treatment and research have meant survival rates are pitiful – with only 4% of patients surviving for five years as opposed to 87% of breast cancer patients.
The statistics are shocking as an early diagnosis can mean the difference between a tumour that is treatable with surgery and one that isn’t. Almost half of those diagnosed with pancreatic cancer will, like Ivan, get their diagnosis in A&E (compared to just 20% of other cancers). ‘By the time they get to A&E they’re showing classic symptoms of weight loss, abdominal pain and jaundice and their disease is often at a late stage,’ says Prof. Pippa Corrie, consultant and associate lecturer in medical oncology at Cambridge University Hospitals NHS Foundation Trust.
In its early stages, the disease is often misdiagnosed by GPs as conditions such as gall stones, Irritable Bowel Syndrome, gastritis or hepatitis, she says. In fact, one in three pancreatic cancer patients need three or more visits to their GPs before being referred to specialists and a 2012 study found that 49% of GPs didn’t feel confident spotting the signs – albeit vague symptoms – such as back pain, upper abdominal pain, skin itching or gastric changes (especially oily, floating poo) which are all signs that investigations are called for.
For Jade Currell, it took five months of to-ing and fro-ing with doctors for what began as back pain then turned into a sharp, radiating gnaw in the centre of her stomach before she finally received a devastating diagnosis of advanced pancreatic cancer – also in A&E. She was 27. ‘The consultant sat there shaking his head while I sat there numb trying to calm down my mum and boyfriend,’ Jade, a former dementia care worker remembers.
‘It was January and since the previous August I had been investigated for meningitis, gall stones and had had every blood test going, but I wasn’t expecting this. I kept asking the consultant ‘How long have I got?’’ Jade was given chemotherapy but her cancer had already spread to her liver and was inoperable.
‘I’ve handled treatment so well, the doctors who gave me initially three to six months to live, now don’t know how long I have,’ says Jade. ‘I’m not going to let cancer stop me living life, it’s just a word’.
‘The vast majority of pancreatic cancer patients are diagnosed with pancreatic cancer after age 60 so most doctors won’t be looking for this diagnosis in a 27 year old,’ says Prof. Corrie. ‘Still, we need to be aware because there is a group of young people like Jade who will contract the disease so people need to know the signs, seek help early and for GPs to listen to their patients and refer them.’
Though it also took Ivan five months to get a diagnosis (after being told his stomach pain was acid reflux) his tumour, which measured 30 millimetres, was at the head of his pancreas, making him eligible for a Whipples operation. This complicated high-risk surgery is used to treat 10-20% of pancreatic cancers. ‘I like to think of myself as a realistic optimist,’ remembers Ivan. The oncologist explained that the procedure came with a one in ten chance of dying either on the operating table or not recovering and a five per cent chance of surviving up to five years, even if it were successful.
‘I was with my wife Judi and after that meeting I burst out laughing,’ says Ivan. ‘Judi said to me: ‘What are you laughing at?’ and I said: ‘Well, you’ve got to be one heck of an optimist to think that had a bright side.’ Still, Ivan agreed, meanwhile checking his will and life insurance. After having the procedure in December 2011, which took seven hours, he responded well to both surgery and post-operative chemotherapy and his cancer hadn’t spread.
Ivan has since run two marathons and ten months later, was back at work leading a team of 120. ‘I’ve yet to shed a tear over cancer,’ he says. ‘I had to give control to other people, the medics and surgeons and so far they have been incredible. My advice is if you are told one thing, but feel deep down it’s something more serious, get a second opinion.’
But for the 80% of patients for whom surgery won’t be an option, more investment into treatments is desperately needed. Just one per cent of cancer research and treatment money is spent on pancreatic cancer which kills twice as money people as ovarian cancer, but gets only a third of the funding.
Even where treatments do exist, they may not be available. Recently, the drug Abraxane, proven to provide advanced pancreatic cancer patients with at least two and half months prolonged life was taken off the Cancer Drugs Fund in England by the National Institute of Clinical Excellence (NICE), despite being available to patients in Wales and Scotland. If Jade’s current chemotherapy drug stops working, Abraxane will be her only option, but she will face an estimated £5035 bill for a three month round of treatment.
‘It makes me angry that there was a plan B for me in place and now there isn’t,’ says Jade. ‘When you’re going through this, you shouldn’t have to fight for the drug that is going to keep you alive to do the things you want to do and spend the extra time with your family – I wish whoever made those decisions could see how much I want more time to enjoy the moments I have got left with my family and friends’ “.
********************************************************************************
Making a donation. Donations can be made;
• Directly to the Administration address shown on page 1.
• By direct transfer to our bank account at:
HSBC. Sort code; 40-26-07. Account number; 81635190.
Please quote your name as the reference.
• By donating online by credit or debit card with either;
MyDonate at www.mydonate.bt.com or
Justgiving at www.justgiving.com/rbpcr/donate or
Virgin Money Giving at www.virginmoneygiving.com.
They all reclaim Gift Aid for us.
• Leaving a Legacy in your Will. If you want to know more about leaving a legacy, please visit our web site at www.ralphbatespcr.org.uk.
• Gift Aid. If you are a UK tax payer we can claim 25p from HMRC for every £1 you donate. You can download a Gift Aid declaration from our web site but no need to do this if you donate through one of the web sites named above. They take care of Gift Aid. But you must have paid or will pay an amount of Income Tax and/or Capital Gains Tax for each year (6 April to 5 April) that is at least equal to the amount of tax that all the charities or Community Amateur Sports Clubs that you donate to will reclaim on your gifts for that tax year. VAT and Council Tax do not qualify.
*****************************************************************************

